Flatfoot Conditions
What is an Adult Acquired Flatfoot Deformity?
Adult Flatfoot Deformity is a condition of the foot where the arch on the inside of the foot collapses to the ground after previously being normal. This is also known as “fallen arches” or medically as Pes (Foot) Planus (Flat).
Should I have my Flatfoot corrected?
If you have tried physiotherapy, anti-inflammatories and arch supports and your flatfoot has constant pain and restricts your everyday activities you should seek a surgical opinion.
Who gets Flatfoot?
Not all flatfeet are the same. The most common type is usually present from birth and normal. Approximately 30% of the general population have a form of this flatfoot with the majority affecting both feet and remaining pain free.
A painful flatfoot usually occurs in adults who have had a previously normal arch and acquire the deformity over time. This usually occurs in females and is more prevalent during middle age however can also happen in men and younger patients.
Book an Appointment Today!
What are causes of Adult Acquired Flatfoot Deformity?
The most common cause of Adult Acquired Flatfoot Deformity is a torn or degenerate posterior tibial tendon. This tendon goes down the inside of the leg and is important in maintaining the arch while walking. However, as it fails, pain develops along the tendon and with repetitive load the arch of the foot begins to fall and the severity of the deformity begins to increase.
The exact cause of tendon failure is unknown however previous trauma, obesity, high blood pressure, diabetes, increasing age, corticosteroid use, and rheumatoid arthritis increase your risk of developing the condition.
What are the symptoms of Adult Acquired Flatfoot Deformity?
- Pain and swelling around the ankle and foot.
- Inability to walk long distances and tip toe.
- Tired and sore feet with prolonged activity.
- Difficulty and discomfort with shoe-wear.
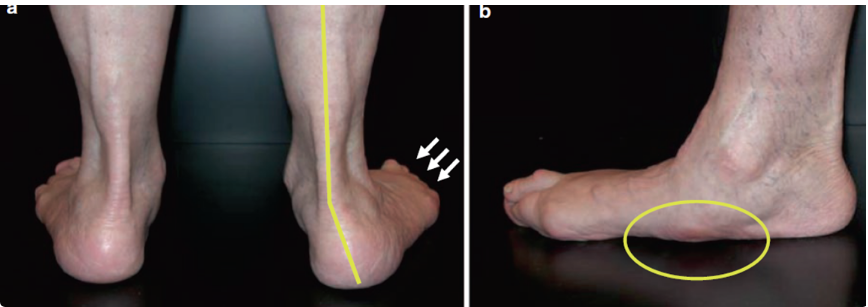
- Change of shape of the foot with a loss of the arch and the toes pointing outwards.
- Inability to to weight bear on affect foot and difficulty with prolonged standing or walking.
What other Conditions are associated with a Flatfoot?
Bunion – Painful bony bump that develops on the inside of the foot at the big toe joint.
Tarsal Coalition – abnormal connection between bones in the foot.
Rheumatoid Arthritis – autoimmune disease that causes painful swollen joints.
Ligamentous Laxity – condition in which the ligaments of the body are loose.
How do you Diagnose Adult Acquired Flatfoot Deformity?

Dr. Chow will take a thorough medical history to delineate the nature of the pain, evaluate the degree of functional impairment and assess the deformity. Risk factors such as Rheumatoid Arthritis, diabetes and any other significant medical history will be considered. Diabetes and cigarette smoking greatly reduce the healing capability of any surgery and increase the risk of infection.
A physical examination will be undertaken to evaluate the flexibility of the foot and isolate any other areas of pain and tenderness in the foot and ankle.
Imaging is essential to evaluate the severity of the deformity and associated degeneration. Weight bearing x-rays of the foot and ankle are reviewed for evidence of osteoarthritis and the bony alignment of the foot. An MRI is also required to assess the quality of the tendon and surrounding soft tissue.
